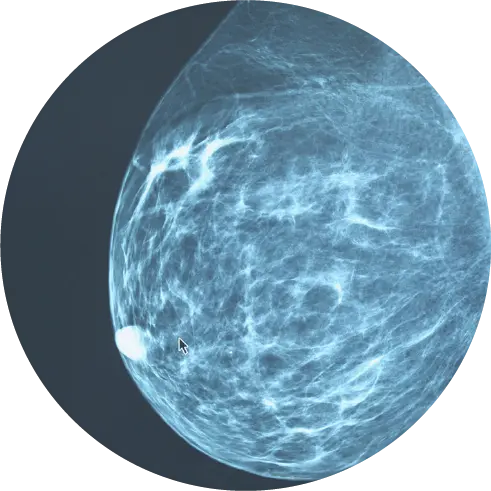
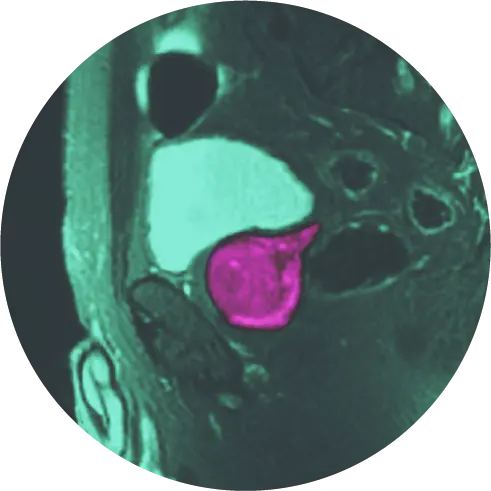
When prostate cancer is suspected, a biopsy is needed to confirm?or rule out?a cancer diagnosis. During a biopsy, a needle is inserted into the prostate gland through the wall of the rectum. A small amount of tissue is removed and sent to a laboratory for further evaluation.
The vast majority of prostate biopsies are trans-rectal ultrasound (TRUS) biopsies. Unfortunately, these are imprecise and expose men to an assortment of unpleasant side effects including infection, rectal bleeding, urinary problems (frequent urination, weak or slow stream or dribbling urine) and sexual dysfunction.
A typical TRUS biopsy only samples tissue from 1% of the prostate gland. The ultrasound used to guide the needle is unable to distinguish between healthy and cancerous tissue, which means the biopsy will be random and ?blind.? As a result, in as many of 20-30% of cases, clinically significant cancers were completely missed, leading to false-negative diagnoses. Additionally, aggressive treatment resulted in about half of all cases when cancer was detected but the TRUS biopsy?s limitations failed to accurately characterize slower-growing lesions as non life-threatening. 1
When cancer is missed, other testing (such as PSA) or symptoms experienced by the patient may indicate a growing concern, requiring more biopsies. It is not unusual for a second or third biopsy to be performed?each time returning negative results?while undetected cancer in the prostate gland continues to grow. Unfortunately, this can lead to a late-stage diagnosis and the higher likelihood of treatment failure.
There is a newer and more precise biopsy option, and it?s growing in popularity among patients and their doctors. MRI-guided biopsy uses high-field MRI to help the doctor guide the biopsy needle more precisely to the area of concern inside the gland. It carries less risk for the patient than a TRUS biopsy, as well as fewer side effects.2.3
Multiparametric prostate MRI (mpMRI) is now used as a front line screening test, and is recommended by the American Urological Association to be performed before a prostate biopsy. In many cases, it can show the size, shape and characteristics of a prostate lesion, and can help doctors to understand how aggressive the cancer may be. If the mpMRI reveals potential cancer, the same technology can then be used to guide the biopsy in real time. This ensures sampling from only the most suspicious areas, reducing the need for more ?needle sticks? as well as the need for repeat biopsies and their associated side effects.
MRI-guided biopsy is an option for all men with suspected prostate cancer. It is performed on an outpatient basis at HALO Diagnostics. If you?ve been told you need a biopsy, we encourage you to call us at 760-469-8057 to learn more about our MRI-guided prostate biopsy options.
To schedule a complimentary case assessment and have a HALO Diagnostics team member contact you, click the button below:
(1) Tareen B, Godoy G, Sankin A, et al. Can contemporary transrectal prostate biopsy accurately select candidates for hemi-ablative focal therapy of prostate cancer? BJU Int. 2009 Jul;104(2):195-9.(2)Giganti, Francesco and Moore, Caroline M.Transl Androl Urol. 2017 Jun; 6(3): 432?443.
(3)Egbers N, Schwenke C, Maxeiner A, Teichgräber U, Franiel T. MRI-guided core needle biopsy of the prostate: acceptance and side effects. Diagn Interv Radiol. 2015;21(3):215-221. doi:10.5152/dir.2014.14372