Laser Prostate Surgery
Using Laser Focal Therapy (Focal Laser Ablation)
Laser Focal Therapy (LFT) Prostate Cancer Surgery
We use Laser Focal Therapy (focal laser ablation) for the treatment of low-to-intermediate prostate cancer. This prostate laser surgery can also be used to help improve the symptoms associated with benign prostatic hyperplasia (BPH).
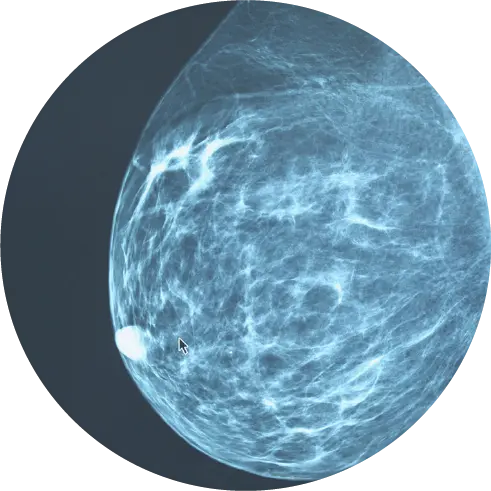
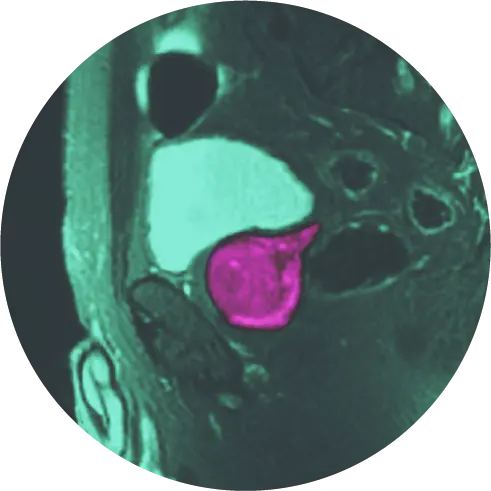
This procedure involves placing the patient inside the MRI scanner and displaying MRI images and thermal maps on a computer screen. A thin laser fiber is guided to the tumor and laser energy is applied to ablate, or kill, cancer cells.
The temperature and the extent of the ablation zone are constantly monitored with MRI imaging, allowing HALO Dx clinicians to determine if all visible tumors have been destroyed.
Laser Focal Therapy has demonstrated hugely successful results2:
- < 1% erectile dysfunction compared to about 50% with whole gland prostatectomy
- < 1% incontinence compared to over 25% risk with whole gland prostatectomy
Committed to Progress
Dr. John Feller, Chief Medical Officer at HALO Diagnostics, recently presented 10-year results from our phase II clinical trial of laser focal therapy for prostate cancer. The results are impressive.2
| 100% | Prostate cancer survival rate. |
| <1% | Erectile dysfunction compared to ~50% with whole gland prostatectomy. |
| <1% | Incontinence compared to over 25% risk with whole gland prostatectomy. |
| <1% | Infection compared to 4% with whole gland prostatectomy. |

Advantages
of Laser Focal Therapy (Focal Laser Ablation) Surgery for Prostate Cancer Treatment
MINIMALLY INVASIVE
Minimally invasive, ambulatory outpatient procedure – usually a 4 hour procedure.
Rapid Recovery
Most patients can return to work the next day.*
NO ANESTHESIA
No general anesthesia required.
IMPROVED URINATION
Vast majority of men have improved urination after the procedure.*
LOWER RISK OF SIDE EFFECTS
Lower risk of side effects such as urinary incontinence, impotence and decreased bowel function compared to surgery or radiation therapy.
IMPROVED ACCURACY
Better accuracy compared with other focal approaches, e.g. High-Intensity Focused Ultrasound (HIFU).
NO LIMITATIONS
Unlike other treatments, focal laser therapy does not limit the option to treat with radiation therapy or surgery if needed later.
Radical Prostatectomy and Other Traditional Prostate Cancer Treatment Procedures Can Have Severe & Permanent Side Effects
- 50% risk of erectile dysfunction (impotence).
- 25% risk or urinary incontinence.
- Dry orgasm.
- 20-40% cancer recurrence within 10 years, 30-50% cancer recurrence during patient’s lifetime.
Laser Focal Therapy
Invented by HALO Diagnostics
In 2010, the team of Bernadette Greenwood, Chief Research Officer at HALO Diagnostics, and Roger McNichols, PhD, developed the system to perform Laser Focal Therapy. The first case in the world was performed by the HALO Diagnostics team of Dr. John Feller, Ms. Greenwood, and Dr. McNichols in 2010.
HALO Diagnostics released interim 10-year results from its Phase II 20-year clinical trial for prostate laser focal therapy in patients with localized prostate cancer. Over 170 men, 45-years or older diagnosed with low-to-intermediate risk or recurrent prostate cancer, volunteered to participate in the study. The results are impressive: less than 1% infection, less than 1% erectile dysfunction and less than 1% incontinence – compared to conventional whole gland prostatectomy which has a risk of up to 50% erectile dysfunction and 25% urinary incontinence. These results, along with a 100% prostate cancer-specific survival rate, are an encouraging development for men looking for a prostate cancer therapy option with a lower risk of side effects.
Featured Patient Testimonial: Dr. Terry Higgins
After receiving a prostate cancer diagnosis, Dr. Terry Higgins’ urologist warned him of the risk of side effects of standard-of-care prostate cancer treatments like a radical prostatectomy, which carries a 50% chance of causing erectile dysfunction, and a 25% chance of causing incontinence.
At just 53-years-old, those were odds that Dr. Higgins was not willing to accept. Dr. Higgins’ urologist then told him about laser focal therapy, a minimally invasive prostate cancer treatment pioneered by HALO Diagnostics.
Now a few years in remission, Dr. Higgins shared his story.
Featured Patient Testimonial: Dr. David Mantik
“As a physician speaking to a patient, I have on a number of occasions disclosed to them that I myself had prostate cancer and actually had this procedure and I highly recommend it for the appropriate candidates.”
Dr. David Mantik is a radiation oncologist. For more than 40 years, he’s specialized in the use of radiation therapy to treat patients with prostate cancer.
However, at the age of 79 when he noticed his PSA (prostate-specific antigen) score was rising, Dr. Mantik went to see Dr. John Feller. Now in remission, Dr. Mantik shared why he chose laser focal therapy over radiation treatment for his prostate cancer.
Featured Patient Testimonial: Tom’s Story
“I just felt like the technology and the skill level of HALO Dx was light years ahead of what was here available to me locally and that’s why I made the choice to go down there. It just seems like a rational, logical alternative that you don’t have to be a doctor to be able to appreciate.”
Featured Patient Testimonial: Wayne Gregory
Family, safety, and preserving quality of life were top of mind for Wayne Gregory when he chose laser focal therapy, also known as focal laser ablation (FLA), to treat his prostate cancer.
“I had lesions ultimately on both sides of the prostate near the nerve bundles,” said Gregory. “I knew that the skill and precision it was going to take to get that cancer ablated was going to have to be very, very high.”
He shared his story while on a trip back to Houston, Texas, where he had the procedure performed by Dr. Ara Karamanian, Director of HALO Diagnostic’s Prostate Program and Medical Director of the Prostate Laser Center.
Laser Focal Therapy: What to Expect
You will receive both email and phone contact information for our medical team so that you can always reach us. In addition, we conduct a pre-operative consultation prior to the procedure, we meet the day of the procedure, and will see you frequently in follow-up.
Our team will have collected and reviewed your medical records to evaluate you for inclusion and suitability. Our surgical team will have discussed your case during Tumor Board and conducted a surgical plan based on size, number, shape and location of ablation areas. Prior to the procedure, we will review the Informed Consent Document with you to ensure you understand every aspect of the procedure. We will discuss the risk, benefits, and paperwork of the procedure.
The day of the procedure, our nurse will place an intravenous catheter (IV) in your arm so that she/he can administer IV antibiotics, pain medications and fluids (to maintain hydration). Should other medications be necessary, they will be administered through this IV as well.
You may have a urinary catheter placed so that we can provide cooled urethral saline through Continuous Bladder Irrigation (CBI) protection. This catheter remains in place depending on the size, shape, and location of treatment. Our urologist will perform the insertion and removal.
Patients are positioned on their stomach on the MRI table for the procedure. A small rectal probe (the diameter of an index finger in width) covered in numbing lidocaine jelly to allow access to the prostate. We use the transrectal route for laser fiber placement. This is minimally invasive (compared to thermocouples and transperineal needles), with fewer complications and less recurrence. Technical errors due to misregistration are also less frequent with transrectal fiber placement under MRI guidance.
During the procedure, we will use real-time MRI to visualize the target, guide placement of the laser fiber, and ablate (destroy) cancer cells or for either cancer or BPH (an overgrown transitional zone) while protecting healthy tissue with “safety markers” that are positioned at the urethra and neurovascular bundle. This helps monitor sensitive structures to decrease risk of damage to urinary and sexual function.
Patients will return home or to their hotel room after at least two hours in the recovery room that same day. They must be accompanied by a family member or care giver as driving is not permitted.
We see each patient again according to our rigorous follow-up protocol. This includes follow-up imaging, biopsy and PSA monitoring.
At HALO Dx we are mindful of the patient experience and acceptance of the technology. We do not offer endorectal coil for MRI for the same reasons, instead, we offer a high channel-count phased array pelvic coil. This surface coil is used for both diagnostic prostate imaging and allows access to biopsy and therapy.

Schedule a Consultation
Submit this form and we will contact you, usually within 24 hours, to answer your Prostate screening, diagnosis, and treatment questions.