BPH Overview & Prostate Enlargement Treatment
Benign Prostatic Hyperplasia Overview
Benign prostatic hyperplasia (BPH), also called prostate gland enlargement, is common as men age into their late forties and beyond. An enlarged prostate can cause bladder, kidney and urinary tract problems and may lead to several uncomfortable urinary symptoms, including:
- Frequent and more urgent need to urinate
- Waking up at night to urinate
- Weak urine stream
- Difficulty and straining to empty the bladder
- Delayed onset of urination
- Inconsistent urine flow

Effects of an Enlarged Prostate
The prostate is a small, nut-sized gland that is part of the male reproductive system located in front of the rectum, between the bladder and the penis. The prostate releases a milky fluid which is a key ingredient of semen.
The bladder and urethra are essentially a pump and a tube. When the prostate enlarges, it will often create pressure against the tube (the urethra), causing resistance to urine flow. The bladder must then pump harder to push urine out against resistance. Eventually, the bladder can no longer empty, and the urine that remains in the bladder is known as the post void residual. Generally, once the post void residual is greater than 50 cc or mL, there is irreparable harm being caused to the bladder. Treatment can help partially reverse bladder damage, prevent further damage and help improve uncomfortable urinary symptoms.
The post void residual urine, urine that remains in the bladder after urinating, is essentially stagnant urine that provides bacteria a good environment to grow and a urinary tract infection to develop. Therefore some men who previously never had a urinary tract infection (UTI) can start to get them after developing BPH.
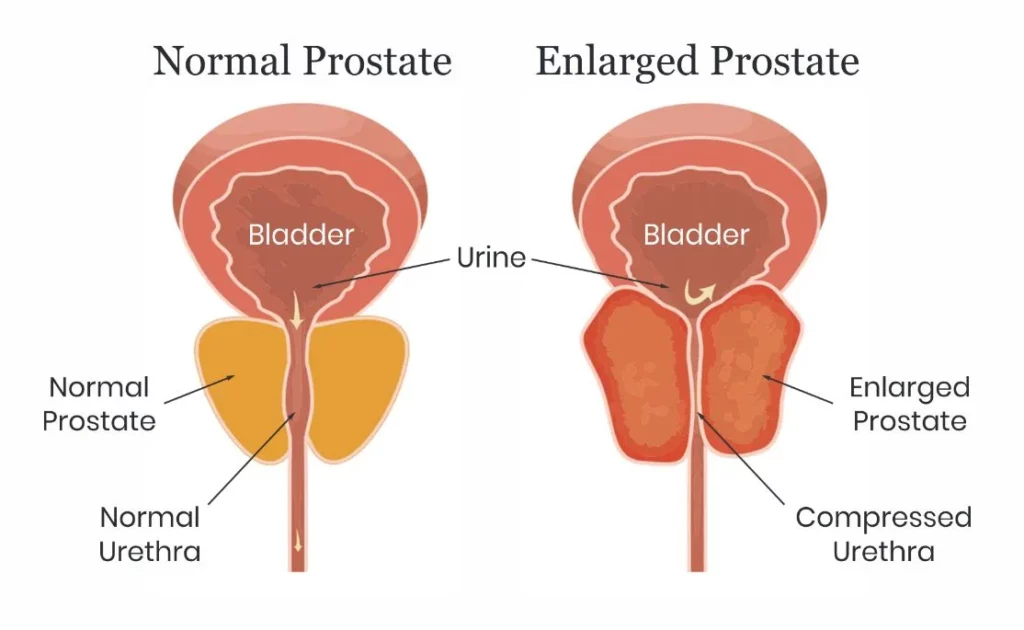
Benign Prostatic Hyperplasia
Cause and Risk Factors
The prostate gland can enlarge as men grow older. The exact reasons for continued growth are unclear but may be related to changes in sex hormones as men age. While the exact cause(s) of BPH or an enlarged prostate remain unclear, there are risk factors that are important to keep in mind, including aging, family history, obesity and underlying conditions that may increase the risk of BPH like diabetes and heart disease.
Diagnosis
Your doctor will ask detailed questions about your symptoms and usually perform a physical exam. Typically, the following exams and tests may be performed:
- Prostate-specific antigen (PSA) blood test
- Digital rectal exam
- Urine test to help rule out infection or other conditions with similar symptoms
- Blood test to identify potential kidney problems
Additional tests may be required to confirm an enlarged prostate and rule-out other conditions:
- Post void residual volume test to help determine if you can empty your bladder completely
- Urinary flow test to measure the strength of urine flow
- You may be asked to record the frequency and the amount or urine in a 24-hour voiding diary
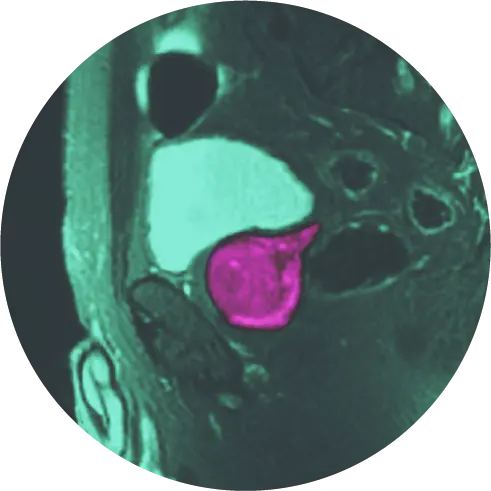
In some situations, and in more complex conditions, your doctor my recommend imaging using ultrasound or MRI to measure and evaluate your prostate or perform a biopsy to rule-out prostate cancer.
The Problem With Traditional BPH Treatment
One of the most popular approaches is a procedure called transurethral resection of the prostate (TURP). Also known as a “roto-rooter” due to the approach of widening the urethra and urinary sphincter, TURP was first performed in the United States in 1926. While there have been advances in this treatment technique, it is still very invasive. The average blood loss from a TURP is 500 cc (half a liter), and it requires a hospital stay. A camera and cutting device are advanced into the penis. The prostatic urethra and the internal urinary sphincter are carved out and the urologist will continue cutting out tissue until he or she feels an adequate amount has been removed. While this is an effective procedure, approximately 90% of men may have retrograde ejaculation and approximately 5-10% of men can experience erectile dysfunction at some point following a TURP.
Because of the large amount of blood loss associated with TURP, GreenLight laser was developed. It is very similar to a TURP, except that instead of using a cutting device, a very high-powered laser is used to literally vaporize the prostatic urethra and tissue beyond.

BPH Treatment With Laser Focal Therapy
A PROCEDURE PERFORMED PRECISELY
To help minimize the risks of BPH treatment, HALO Diagnostics uses a laser system to insert a very thin (1.85 mm) laser fiber through the rectum into the prostate under MRI guidance. By monitoring the laser energy in two different planes in real-time using MRI, HALO Diagnostics’ physicians can visualize important structures near the prostate, including the neurovascular bundles (the nerves responsible for erectile function) and the ejaculatory ducts. This laser system is so precise, that its most common use is in the brain. While there are no guarantees in medicine, risks to the neurovascular bundles, internal urinary sphincter, and prostatic urethra can be minimized with the HALO Diagnostics’ approach. With this treatment option, the risk of retrograde ejaculation is less than 10% and the risk of erectile dysfunction is minimal.
AFTER THE PROCEDURE
Because we do not carve through the underlying anatomy, but rather ablate the excess tissue, initially patients’ urinary function gets worse before it gets better (due to swelling). This is why our BPH patients will keep the urinary catheter in for a week after the procedure. Most men return to baseline urinary function in three weeks and have significant improvement 6-8 weeks following the procedure.
Treating BPH With TULSA-Pro
TULSA-PRO has proven to successfully treat BPH with no incisions, radiation, and with a lower risk of side effects.
TULSA-PRO is an effective option for men with BPH as it destroys enlarged prostate tissue while avoiding damaging vital structures. The procedure is completed in one treatment session and performed under general anesthesia.
Learn more about the TULSA-Pro procedure for BPH.
Schedule a Call
Submit this form and we will contact you, usually within 24 hours, to answer your Prostate screening, diagnosis, and treatment questions.
1.https://www.cancer.org/cancer/prostate-cancer/about/key-statistics.html
2.https://zerocancer.org/learn/about-prostate-cancer/risks/african-americans-prostate-cancer/