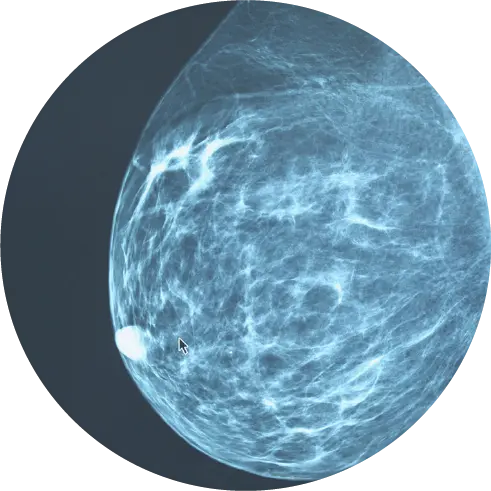
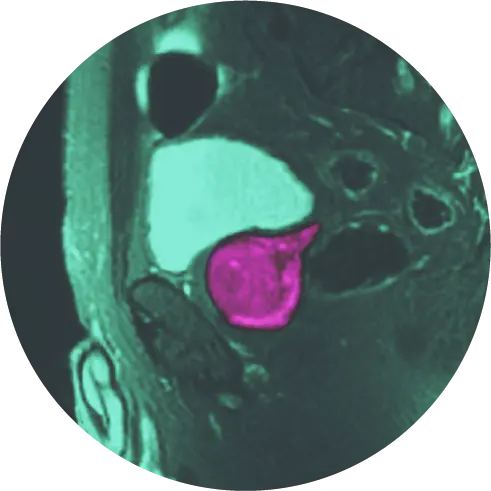
Breast cancer screenings can help detect the disease early when it is easier to treat. However, you may wonder when you should begin getting your screenings and how often you should have them. According to the American College of Radiology (ACR), you should start annual mammogram screenings at age 40 and consider starting earlier depending on your risk factors and family history.1 HALO is here to help you determine what age is best for you depending on your risk factors.
How Different Categories of Risk Influence Your Screening Recommendations
Women of Average Risk for Breast Cancer
A woman who is considered at average risk of getting breast cancer is someone with no family or personal history of breast cancer. Additionally, this individual does not carry a breast cancer gene mutation (such as the BRCA1 or BRCA2 gene mutation) and has not had chest radiation therapy before age 30. Women of average risk are recommended to begin annual mammograms to screen for breast cancer starting at age 40.1
Screenings should continue if you are in good health and expect to live 10 more years.
Women of Moderate Risk for Breast Cancer
A woman who has a moderate risk of getting breast cancer is someone who has not had the disease herself and does not carry one of the breast cancer gene mutations. However, she has a relative—particularly a first-degree family member (mother, sister, or paternal aunt)—who has had breast cancer.
If you fall into this category, you may benefit from starting annual mammograms at age 40, according to the United States Preventive Services Task Force (USPSTF) and the ACR.1 Starting mammograms earlier, decreases the chances of receiving a late-stage cancer diagnosis when survival rates are lower.
Women at High Risk for Breast Cancer
Experts consider a woman to be at high risk for getting breast cancer if she meets one or more of the following criteria:
- She has had breast cancer before.
- Have a calculated lifetime risk of breast cancer >20% based on assessment tools.
- She has a first-degree family member with the BRCA1 or BRCA2 gene mutation.
- She is a known carrier of the BRCA1 or BRCA2 gene mutation (or meets the above criteria and has not been tested for the gene mutation).
- She has a medical condition that increases her risk (such as Li-Fraumeni syndrome, Cowden syndrome, or Bannayan-Riley-Ruvalcaba syndrome).
Having a high-risk designation does not mean you will get breast cancer. In fact, many women have some of the risk factors but never develop breast cancer. However, early detection means tumors and other signs of breast cancer can be discovered earlier when treatment options are often easier and more successful.
The ACS recommends that these individuals begin annual mammograms at age 30 and discuss other steps that meet their individual circumstances with their doctor.2 If you have dense breasts, your doctor may advise getting both a mammogram and a breast MRI for more precise imaging.
In some instances, women with a first-degree family history of breast cancer are suggested to start getting mammograms when they are 10 years younger than the age at which their relative was diagnosed.3
How to Determine Your Risk for Breast Cancer
Health professionals use the National Cancer Institute’s Breast Cancer Risk Assessment Tool to estimate a woman’s risk and age to begin screening. This tool allows your doctor to evaluate your chances of developing invasive breast cancer over the next five years and your lifetime risk as you age.
It uses information involving your personal medical history, including your reproductive history and whether your first-degree relatives have had a breast cancer diagnosis. The main risk factors are ones you cannot control—your gender and your age. Most breast cancers are discovered in women who are age 50 and older.4
The tool is valid for white, black/African American, Hispanic, and Asian and Pacific Islander women in the U.S.; however, it may underestimate the risk in black women with previous biopsies and Hispanic women born outside this country. Also, since research data that is specific to American Indian/Alaska Native women is limited, their risk information may not be as accurate. The tool also doesn’t account for a personal history of some cancers or the presence of the BRCA gene mutations.5
Important Takeaways
Research shows that when you should begin screening depends on a combination of several factors. Talk with your physician to understand your risk and discuss the benefits and risks of beginning screening.
Keep in mind that most women have some risk factors for breast cancer, but most women do not get the disease.
Early detection means tumors and other signs of breast cancer can be discovered when treatment options are likely to be more successful. At HALO Precision Diagnostics™, we offer breast screenings at our HALO Breast Care Center in Chico, Silicon Valley MRI in Silicon Valley, Palms Imaging Center in Oxnard, and Precision Imaging Centers‘ four locations in and around Jacksonville, Florida. Take control of your health today by reaching out to our breast care experts at 877-225-2831 or by filling out the form below!
References
- https://www.jacr.org/article/S1546-1440(17)31524-7/fulltext
- https://www.cancer.org/healthy/find-cancer-early/american-cancer-society-guidelines-for-the-early-detection-of-cancer.html
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7855994/
- https://www.cdc.gov/cancer/breast/basic_info/risk_factors.htm
- https://bcrisktool.cancer.gov/index.html