In 2011, the United States Preventive Services Task Force (USPSTF) issued a grade of “D” to the prostate specific antigen (PSA) test. A “D” grade generally means that the test does more harm than good.
But is that really the case?
Prior to the USPSTF announcement, the PSA test was recommended to all men over 50 and younger men at elevated risk for prostate cancer. The readily available blood test is designed to measure concentrations of the prostate-specific antigen, a protein produced by the prostate gland. An elevated PSA level could be an indication of prostate cancer or due to a benign condition, such as inflammation (prostatitis).
The USPSTF likely issued their recommendation because in the past, many men with elevated PSA were advised to have prostate biopsies. A significant number of these PSA-inspired biopsies turned out to be negative, but not before exposing men to an assortment of unpleasant side effects including infection, urinary incontinence and sexual dysfunction. In other cases, men were over-treated for slower-growing prostate cancers which would not necessarily have been life-threatening.
However, it is not fair to blame these shortcomings of prostate cancer detection and treatment on the PSA test. In fact, the PSA test remains one of the few inexpensive tests that can alert the physician and their patient to a potential problem. It may not be perfect, but it’s what we have until something better comes along.
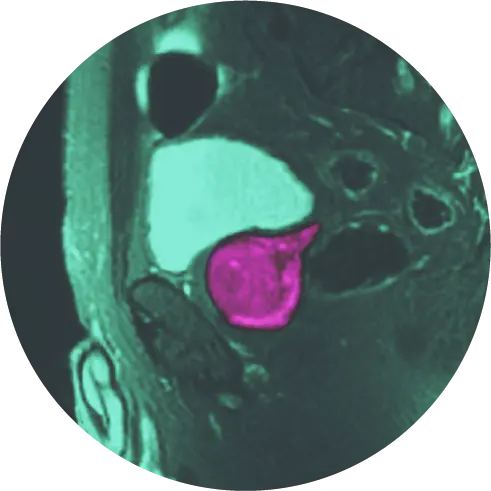
In late 2019, the American Urological Association issued a statement advocating the use of multi-parametric prostate MRI as a front-line test for prostate cancer. For men with an elevated PSA, an abnormal digital rectal exam and/or other risk factors, this test could preempt a biopsy by ruling out cancer (or clinically significant cancer) in a non-invasive fashion. When a biopsy is needed, MRI-guided biopsy is more precise than TRUS with less risk and fewer side effects.1.2
Some claim that the reduction in PSA screening since the USPSTF announcement has led to fewer cancer diagnoses, citing statistics that show a decline in observed prostate cancer diagnoses since 2011.3 But all this means is that when cancer is finally diagnosed, it will likely be at a later stage and more difficult to treat.
At HALO Diagnostics, we use multiparametric magnetic resonance imaging (mpMRI)–combined with PSA testing–for the timely and accurate diagnosis of prostate cancer. Take control of your prostate health today by learning more about screening for prostate cancer.
(1) Giganti, Francesco and Moore, Caroline M.Transl Androl Urol. 2017 Jun; 6(3): 432-443.
(2) Egbers N, Schwenke C, Maxeiner A, Teichgräber U, Franiel T. MRI-guided core needle biopsy of the prostate: acceptance and side effects. Diagn Interv Radiol. 2015;21(3):215-221. doi:10.5152/dir.2014.14372
(3) Source: National Cancer Institute Surveillance, Epidemiology, and End Results (SEER) Program